Over the past few weeks, Dunedin Hospital staff have run a range of real-life simulation exercises for its staff, each re-creating a treatment scenario for a patient with the pandemic disease.
As well as giving clinicians valuable experience, the exercises have had instant benefits for patients and doctors, Otago Clinical Skills Laboratories director Ohad Dar said.
"We had a pathway in the hospital for suspected Covid-19 patients to follow into our Covid-19 area, but after a simulation which threw up a few issues ... we needed to redesign that process.
"A lot of smart people worked on that process, but the simulation uncovered additional issues that needed to be sorted out ... there was a tangible result almost immediately."
The clinical skills department would normally run simulations in individual departments testing out single processes or meeting specific training needs.
Covid-19 offered a rare opportunity, Dr Dar said. Dunedin Hospital being much emptier than usual meant staff were available to take part in inter-departmental simulations, and the need to prepare for possible pandemic cases meant there was an appetite for extra training.
"The simulations are incredibly hard to organise when it’s business as usual, because you have got to compete with service provision for real patients ... this Covid-19 crisis has meant we have had to rethink some of our processes and the simulations are a good way to work through any possible problems."
Over the past few weeks, Dunedin Hospital staff, as well as first responders such as St John and the Otago Rescue Helicopter Trust, have been run through a range of scenarios involving the transfer of a patient with suspected Covid-19 from a rural accident site to the hospital, and then the treatment of that patient in various parts of the building.
"Building up the scenario and building up the backstory for the simulation, sometimes it is inspired by real cases, suitably modified," Dr Dar said.
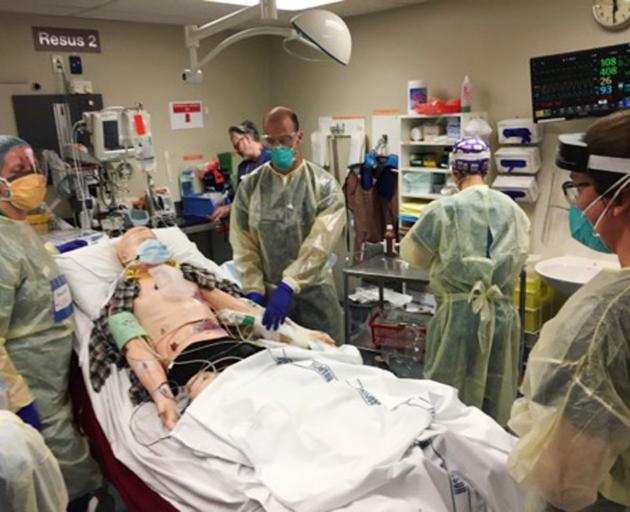
Scenarios have to be realistic enough to focus people’s minds on the training objective, rather than a piece of theatre sports.
However, the story as scripted tends to alter as soon as clinicians start the exercise.
"That’s always the case but I think that demonstrates resilience," Dr Dar said.
"When people have to assess a problem they come up with things you might not expect and you have to work around that. It’s a really interesting part of the simulation because that’s where we can start to learn quality improvement processes."
Quite apart from teaching new skills and checking processes work, often the real worth of exercises came afterwards Dr Dar said, when participants met for a debrief on what worked and what did not.
"At our most recent sim we had paramedics, doctors, nurses, orderlies, radiographers, and staff from various departments like emergency and intensive care and surgery, reflecting on our shared stories and puzzling with issues out.
"It’s good to be able to sit down and share our experiences and have a chat, rather than just meet each other when there is a crisis or a specific medical issue. Training is really good for morale and workplace culture."
Each exercise is documented with a report, a process which senior students at Dunedin School of Medicine have helped with.
All exercise participants kept appropriate physical distancing and wore spare personal protective equipment rather than use the DHB’s reserves.
The exercise was a reminder to staff just how hot and uncomfortable the equipment is, and how it can prevent effective communication, Dr Dar said.
"PPE has its issues; not only is it hot but somehow sound reverberates inside it and that makes it hard to hear — that has come up again and again.
"People have had to come up with communication plans, how do we minimise noise but make sure vital information is passed on to each team member?"












