
It is often said Maori perform poorly in almost all health statistics.
It is one thing to say such a thing but quite another to stare that reality in the face, as the Southern District Health Board did recently.
It asked its chief Maori health strategy and improvement officer, Gilbert Taurua, to write a report on amenable mortality rates for Maori, and earlier this month reviewed his findings in an at times emotional meeting.
"These are our parents, these are our siblings, these are our children," board member Moana Theodore said.
"Tomorrow is the anniversary of my father’s passing and he died of an amenable condition, and if he had had the life expectancy of a non-Maori man or woman he would have seen his grandchildren born, he would have seen the more widespread acceptance and usage of te reo.
"He would have contributed to that, he would have walked me down the aisle, and he would have seen me graduate with my PhD, and he didn’t get that."
Non-Maori have always outlived Maori, a gap which was narrowing until the 1980s, when it started to widen again — in 2016 the Maori rate of amenable mortality was more than twice the non-Maori rate.
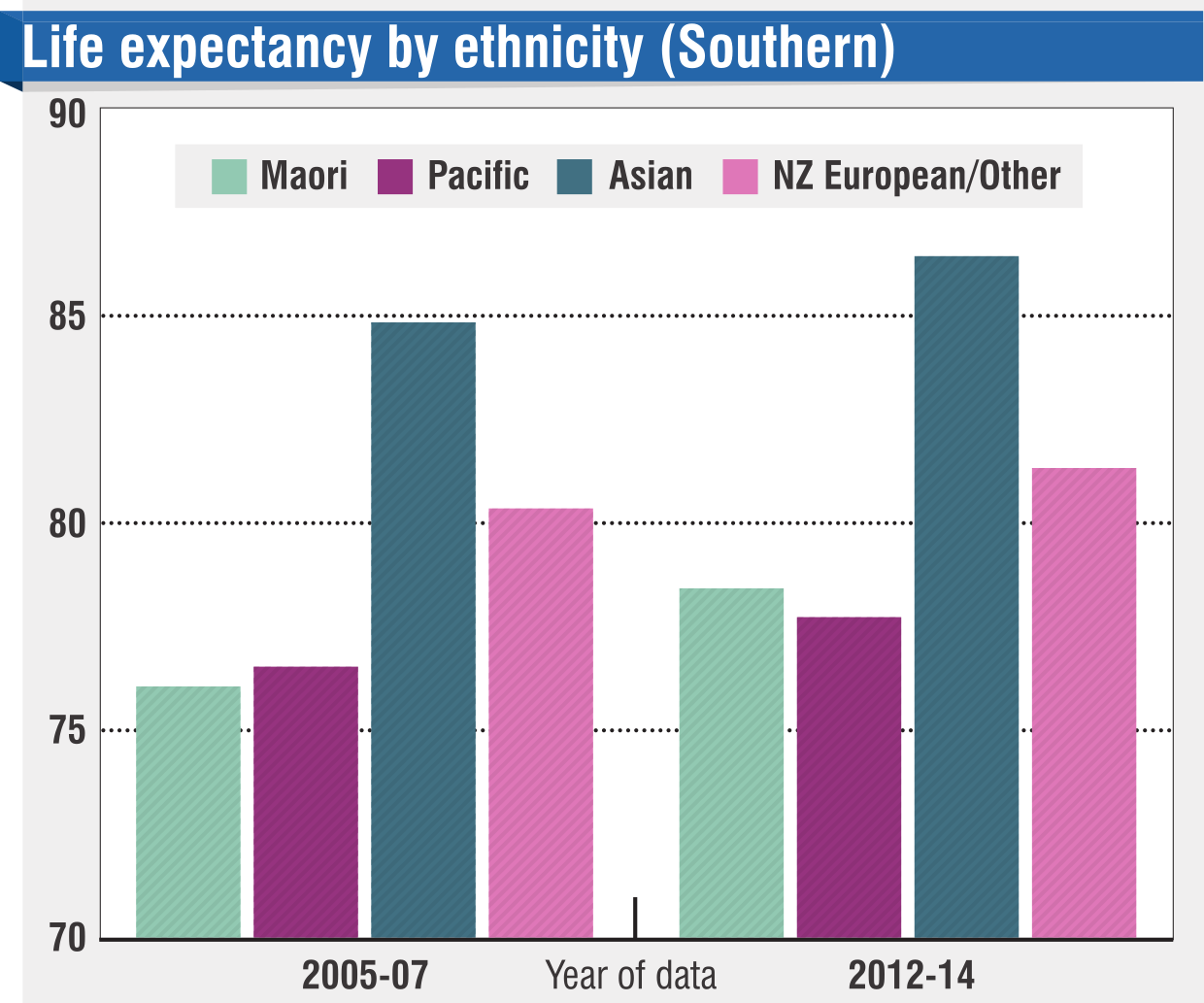
There is a smidgen of good news in the South; statistically Maori live slightly longer here than in many other parts of New Zealand, and between 2007 and 2014 Maori life expectancy increased by about two years, to 78.
But this is all relative — non-Maori life expectancies increased by about the same amount.
A southern Pakeha will live about four years longer than a Maori, and someone of Asian descent can expect to live past 85.
"It was a little bit emotional, although it probably wasn’t telling anybody anything that they didn’t know already," Mr Taurua said.
"Preventable deaths have increased over the years, so things haven’t got better."
The No 1 amenable killer of southern Maori, by an enormous margin, is heart disease.
Suicide is a worryingly high second, followed by respiratory illness and cancer.
"We did a recent audit of our cardio ward in Dunedin and found that Maori patients weren’t coming through those services in any great volume considering the prevalence," Mr Taurua said.
"But we have to think about not only treatment but prevention and the pathways in the community before these people require hospital treatment, so I guess that is a challenge for GPs as well.
"I’m not convinced that all Maori with significant cardiovascular illness are being referred through to secondary services."
While the health service can do much to improve how it cares for Maori, there are other factors at play.
Motor vehicle crashes disproportionately kill southern Maori above other ethnicities, and nutrition, housing and lifestyle choices also add to the amenable mortality picture.
"Tobacco is a major killer of our people and unfortunately we have large numbers of young Maori women who have that tendency," Mr Taurua said.
"Diabetes also underlies
a lot of heart disease."
Board member Tuari Potiki said Mr Taurua’s report should make these issues real for people.
"We all have similar stories about parents and grandparents dying too soon. I have lost half a dozen or more of my best friends — the oldest of us got to 63.
"This is the reality; it is not a theoretical academic paper. It is holes in our whanau; holes that cannot be fixed.
"I am getting tired of sitting in meetings and nodding approvingly of measures, but we do nothing ... Of the boards I have been on this is the one that has been most committed to tackling disparity and inequity, but despite that it feels like we are not doing enough to change it."
So how do things change?
The SDHB, which last year increased its budget dedicated to addressing health inequities, intends to do so again for next year in a budget which has to be confirmed by the Ministry of Health.
Earlier this year the board recommitted to a memorandum of understanding it has with southern runaka to work together to improve Maori health outcomes, and last week it and the ministry signed a further agreement with iwi to work together on the development of the new Dunedin Hospital.
It recently committed to implementing the recommendations of an independent report on its mental health and addiction services, which called for a major budget boost for Maori patients and a genuine commitment to address equity issues.
The Covid-19 pandemic has also strengthened the relationship the board has with Maori, as it has worked closely with kaupapa Maori providers to ensure Maori — who had a far higher per-capita death rate than Pakeha during the 1918 influenza pandemic — are vaccinated at the same rate as all other people.
"I think the relationships have always been relatively strong, but I think that Covid has initiated a greater level of co-operation between the DHB and those providers," Mr Taurua said.
"We have been working seamlessly with them as far as the rollout of the Covid vaccine is concerned, and we sing the praises of our providers because they are able to reach into the more remote areas of our locality more readily than we can, which is a real strength."
Thanks to the Government’s health reforms the SDHB has less than a year left before it is disbanded, but it is determined to do something about Maori amenable mortality before its own demise.
"This is a long-standing issue which has been accepted as part of our New Zealand health system," Dr Theodore said.
"It is unacceptable that we have accepted it, and that needs to change."











