Inaugural professorial lectures have been delivered on marae but it is believed to be the first time in New Zealand one will be made in a country hall.

He is one of 10 hospital staff members who also have teaching, research and administration appointments in the University of Otago’s rural health section.
Prof Nixon is head of rural health in the department of general practice and rural health and is associate dean rural in the health sciences division. He also teaches the postgraduate rural diploma and supervises PhD students.
It was not uncommon for doctors to split their time between research and working in a hospital, Prof Nixon said.
"I don’t think you can be a credible teacher and researcher in health if you’re not doing that."
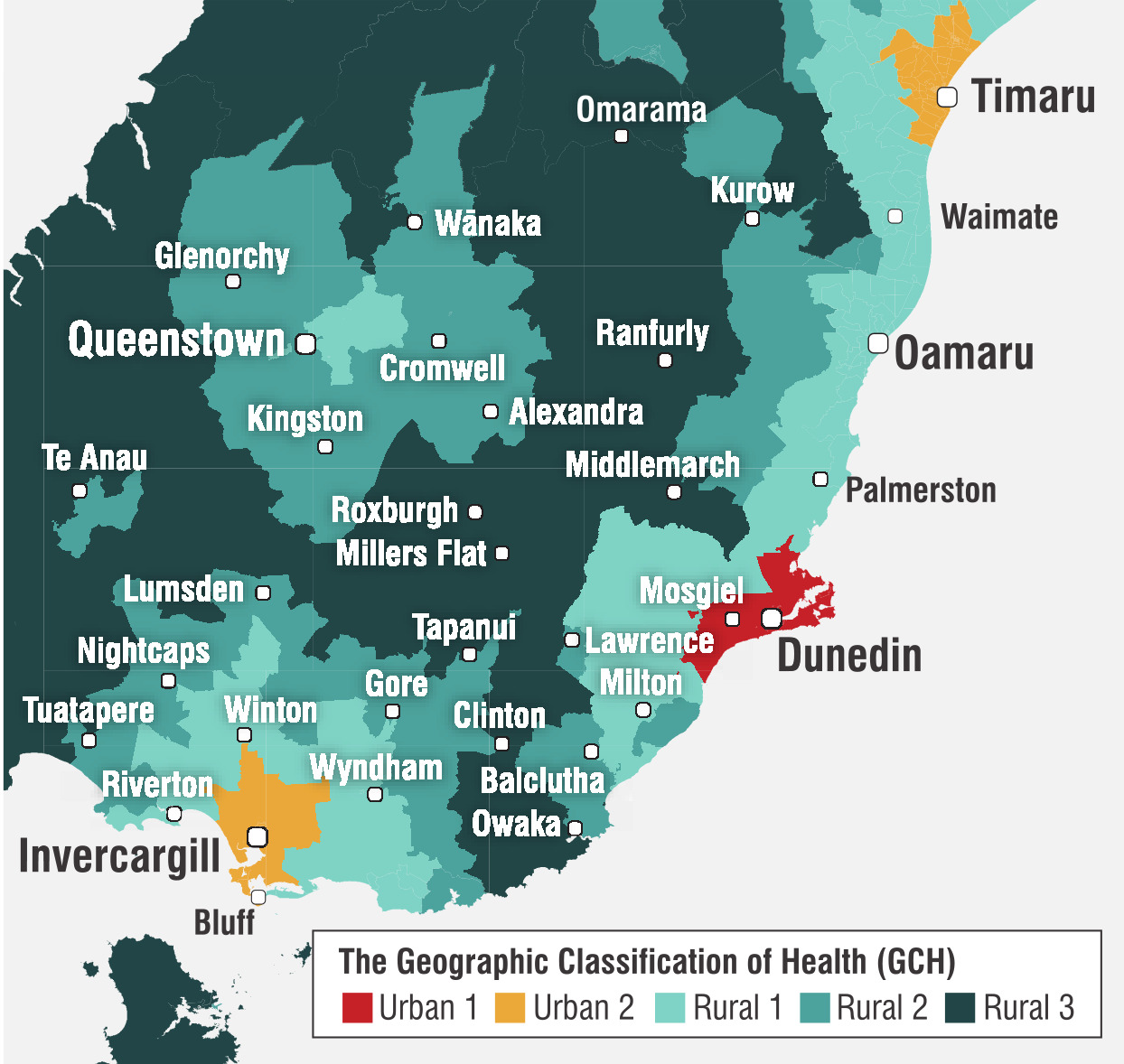
He led a team of researchers who developed a new urban rural classification for health to compare urban and rural health outcomes and access to services.
Prof Nixon’s team developed the geographic classification of health (GCH) with five categories, two urban and three rural, that reflect degrees of reducing urban influence and increasing rurality. The GCH applies these categories to all of New Zealand on a scale from "urban 1" to "urban 2" based on population size, and from “rural 1" to "rural 3" based on drive time to the closest major, large, medium-sized and small urban areas.
The purpose was to find out how healthy rural New Zealanders were compared with city dwellers and how rural people used health services and how good their access to them was, he said.
Historical data suggested the health outcomes for rural and urban people were very similar. However, through teaching and talking with colleagues around the country it was pretty clear that data did not really make sense and was completely different from what was being seen in other countries, he said.
His research explored that in depth and it soon became clear how urban and rural were defined was vague as classification systems were not designed for healthcare and yielded some "silly results".
The GCH had been adopted by the Ministry of Health and the new rural health strategy.
It showed that, like Canada and Australia, health outcomes for rural people were poorer than for urban residents.
Identifying the problem was the first step in solving that problem. The data showed rural people in New Zealand were much less likely to be admitted to hospital than those in the city, which was not the case in Australia and Canada.
"That shows us the rural hospitals that we have left are really important. The communities they’re serving have poorer access to hospitals than people in the city."
Why that was the case was hard to quantify, he said.
"Maybe rural general practice is better at keeping people out of hospital."
But in some cases it could be because getting to hospital was so difficult people did not go. It was likely a combination of factors but it was important to know rural people had poorer access to hospitals.
— All seats for the lecture, that starts at 5.30pm, have been snapped up. It will be livestreamed at: https://www.otago.ac.nz/news/events/inaugural-professorial-lecture-profe...











