His case has prompted dozens of doctors to write an open letter to the prime minister, pleading for change.
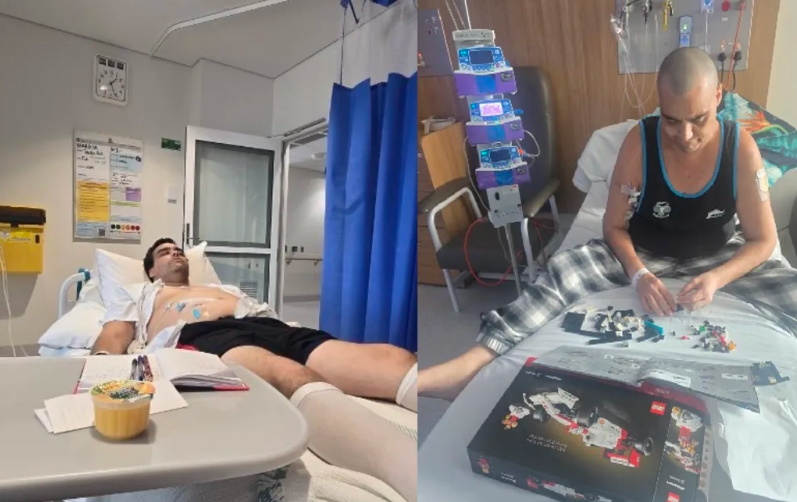
Tawhai Reti was 29 when he was diagnosed with myeloma in 2019.
After going through two stem cell transplants, Reti started on the last funded drug treatment available in New Zealand last year.
But his health continued to rapidly decline, and in December he developed pneumonia and sepsis.
Having exhausted all funded treatment options, he was told he had weeks to live.
The 37-year-old former shearer and his wife then made the difficult decision to leave their family and go to Australia to get drugs that are not funded here.
Reti's wife Lani said they had spoken about moving to Australia in October, but were hesitant about leaving their children behind.
But after his rapid decline, Lani knew it was time to go.
"After a couple of weeks watching Tawhai just lying around, not able to do anything other than sleep and be in pain, I woke up and just realised I couldn't accept it," she said.
"He was dying right in front of my eyes."
Having lived and worked in Australia for a time while he was in remission, Reti still qualified for Medicare cover, and was able access daratumumab - the drug he needed for a chance at survival.
Daratumumab, or dara, is funded in Australia as well as more than 45 other countries, and has been on Pharmac's "options for investment" list for years and is considered a high-priority drug - meaning it would fund it if it had the money.
Reti received his first dose of dara last week, something Lani said was a long-time coming.
"I can't tell you how many tears we had when we found out that he was accepted for dara.
"It's something that we've been fighting for such a long time and trying to spread awareness about and writing letters to the government to try and push for this so that we didn't have to leave home. And within four weeks of being in Australia, he received his first dose."

The pair had to leave their four children at home in New Zealand with Reti's sister.
In order for Reti to reach remission he will need to remain in Australia for at least a year, if not more.
He said being away from his children had been "horrible".
"We've always sort of been a pretty close family... I see them every day, every night, every morning, know everything about them. Now it's sort of just on the end of a phone."
Fundraising done by the family through a Givealittle page helped them to travel to Australia, while still looking after their bills back home.
But now the money was running out.
"We have a mortgage, we have bills like everybody else, we also have four children at home.
"Sadly, I do have to come home. I am leaving next week and Tawhai will have to stay here by himself so I can come home and go back to work to help fund both our home and needs at home and [help] Tawhai stay here."
Tawhai and Lani's family have now set up another Givealittle page to help with their everyday expenses while Reti is in Australia.
'Unnecessary loss of Kiwi lives'
Professor Judith Trotman, a New Zealand-trained haematologist working in Sydney, co-ordinated the open letter from 35 doctors, nurses and clinician researchers.
"We note with alarm the unnecessary loss of Kiwi lives," it reads, because patients are deprived of access to treatments that are available globally and also missing out on clinical trials.
Trotman is treating Reti, who suffers from myeloma, a form of blood cancer which disproportionately impacts Māori and Pacifica patients. Improving survival rates rested solely on access to drug treatments.
"I commend my patient and his wife on their grace and tenacity in facing this painful, progressive cancer. Having for so long been champions for New Zealand's myeloma community, we now focus on his survival and recovery after his immunochemotherapy."
Trotman said the "medical migrants" heading to Australia highlighted the fact that without access to medicines, they will die.
Meanwhile, doctors feel disempowered.
"The lack of modern medicine and technology access and the inability to run many clinical trials are key factors driving highly trained professionals away from New Zealand or prohibiting their return," according to the letter.
A three-point plan put to the government calls for more funding for medicines that are considered 'standard of care' overseas, pointing out that only 0.4% of New Zealand's GDP is spent on medicines, compared to the OECD median of 1.4%.
It also seeks a taskforce of experts to address blood cancer treatment in Aotearoa and asks for more support for research and development to make the country ''a credible and competitive destination for clinical trial research".
The blood cancer specialists - backed by the Australasian Leukaemia Lymphoma Group and the Haematology Society of Australia and New Zealand - say Kiwi patients were also being left behind in accessing clinical trials.
"For these trials to return to New Zealand, access to what are now global standard-of-care comparator drugs is critical."
Auckland haematologist Dr Rory Bennett was one of 35 healthcare professionals who signed the letter.
He said he was disturbed by the state of blood cancer therapy in New Zealand.
"We feel that there's a clear gap between the standard of care that we can deliver here in New Zealand compared with what is achieved overseas, and that gap that is well established is continuing to widen.
"We are very worried about the future of blood cancer therapy in New Zealand and the welfare of New Zealanders with blood cancer."
Bennet said he was frustrated by the situation, but ultimately it was about the patient, not the doctor.
"We find ourselves in difficult circumstances frequently and I feel incredibly sympathetic and sorry for the patients that we have that had they had they lived overseas would have been able to access a more successful or less toxic or frankly just even a therapy that wasn't available in New Zealand.
"Those are hard conversations to have, but it's not about us. It's about the patients at the end of the day and what they are missing out on. And I think that that's the hardest thing."
He hoped that the letter will push the prime minister to work with healthcare professionals on moving blood cancer treatment forward.
"Engage with us... acknowledge the data, hear us out, work with us to try and work this through.
"We're in a desperate, desperate state at the moment, New Zealanders are dying prematurely from blood cancer and we need to sort it out."
'Take us seriously and start listening'
Reti said the letter has left him with no words.
"It just blows me away every time."
Lani hoped that after all their years of crying out for help, the letter will push the government into action.
"I really ask them. to take into consideration the 21,000 blood cancer sufferers in New Zealand that are dying every day because of the lack of funding, because of the lack of standard care.
"I would just strongly urge them to take this letter seriously, take us seriously and start listening and putting things in place for people to continue to be able to live long lives."
Health Minister Simeon Brown said in a statement that improving cancer treatment and outcomes was a key priority.
"Last year we invested $27.1 million to expand stem cell transplant services, helping more patients access life-saving treatment sooner. This funding will strengthen the specialist workforce, increase hospital capacity, and upgrade infrastructure to support more timely transplants."
Brown noted that Health New Zealand was actively recruiting for blood cancer specialist roles across the country.
"I encourage doctors currently working overseas who want to make a difference for Kiwi patients here at home to consider these opportunities."













